What a lifetime with dogs has taught me about these silent, fast-spreading threats.
Have you ever known a dog struggling with a tick-borne disease—like tick fever or Lyme? It’s more common than most owners realize. I’ve seen it firsthand, in more than one corner of the world.
When I was a kid, we spent our summers at the cottage, and our beagles roamed the woods freely, chasing rabbits until dusk. Ticks were practically unheard of. You might find one or two during the whole season—if that. And the idea of disease transmission from a tick? Not even on our radar.
Fast-forward a few decades, and the story looks very different.
These days, finding an engorged tick on a dog isn’t just unpleasant—it’s a red flag. Depending on where the tick came from, your dog could be at risk for a variety of tick-borne diseases, some of which are serious, and in some cases, fatal.
Back when I was training my Labrador Retrievers for field trials, we used to head south every winter—following a route from South Carolina to Tennessee—to visit with friends and get a jump on spring training. I lost count of how many times we found ticks on our dogs weeks after returning to snow-covered northern Ontario. Those ticks had clearly hitchhiked their way north, proof of how easily parasites and pathogens cross borders unnoticed.
More recently, while in Costa Rica, I spent time observing the free-roaming beach and street dogs—many of whom appeared happy and well-adjusted. But I also noticed a few with visible signs of illness. Some were showing symptoms of what I recognized as tick fever (also known as Rocky Mountain Spotted Fever), and many of the dogs at the Playa Samara Animal Rescue were in treatment. It was a wake-up call. I had assumed—wrongly—that tropical beach dogs might be immune to the things we deal with here. The reality is that while freedom suits many of these dogs, access to preventive care and treatment is not a given.
And this isn’t just a Central American issue.
Here in Southern Ontario, tick-borne diseases are on the rise. And while tick prevention products have come a long way, they’re not foolproof. Ticks are sneaky. They hide in fur, between toes, and under collars. They can latch on and go unnoticed for days—even weeks. And once they’re in, so is the bacteria.
In this article, I’m going to walk you through what I’ve learned about the most common tick-borne diseases in dogs—like tick fever and Lyme. We’ll look at how they’re transmitted, what symptoms to watch for, and how to treat and prevent them. Because the earlier you understand the risk, the better chance you have to protect your dog.
Tick-Borne Diseases in Dogs: Common Types, Carriers & Risks
Tick-borne diseases are infections transmitted by ticks that pick up harmful organisms—bacteria or protozoa—when feeding on wild animals like rodents, deer, or birds. When a tick bites and attaches to a dog, it can transmit these organisms through its saliva. Most tick-borne diseases require the tick to be attached for 24–48 hours, though some can be transmitted more quickly. In rare cases, dogs can become infected by ingesting a tick, or through a blood transfusion. Direct dog-to-dog or dog-to-human transmission is extremely rare.
Here’s a simplified, easy-to-read summary of the most common tick-borne diseases in dogs, including the tick species responsible, geographic distribution, typical symptoms, and risks to dogs and humans.
Common Tick-Borne Diseases in Dogs
| Disease | Where Found | Tick Species / Bacteria | Common Symptoms | Risk to Humans / Other Dogs |
| Anaplasmosis (A. phagocytophilum & A. platys) | Worldwide | Deer tick, Brown dog tick, Western black-legged tick | Joint pain, fever, lethargy, appetite loss, nosebleeds, bruising, red gums | No dog-to-human transmission. |
| Ehrlichiosis (E. canis & E. ewingii) | Worldwide | Brown dog tick (E. canis), Lone Star tick (E. ewingii) | Fever, lethargy, bleeding, enlarged lymph nodes, neurologic signs, kidney issues | Not transmissible to humans. Chronic cases have poor prognosis. |
| Rocky Mountain Spotted Fever (Tick Fever) | North, Central & South America | Rocky Mountain wood tick, American dog tick, Brown dog tick / R. rickettsii | High fever, swollen joints, red spots, lethargy, vomiting, diarrhea | Affects both dogs and humans. Can be fatal if untreated. |
| Lyme Disease (Borreliosis) | North America | Deer tick / Borrelia burgdorferi | Lameness, fever, lethargy, enlarged lymph nodes, increased thirst/urination | No direct dog-to-human transmission. Untreated cases may lead to kidney failure. |
| Babesiosis | Emerging in North America | Various tick species / Babesia spp. | Pale gums, dark urine, jaundice, seizures, swollen abdomen, imbalance | Rarely spreads dog-to-dog (bites, in utero, transfusion). Kennel outbreaks possible with poor tick control. |
| Hepatozoonosis (H. canis & H. americanum) | Southern U.S., Gulf Coast, Mexico | Brown dog tick, Gulf Coast tick | Fever, lethargy, weight loss, muscle pain, hypersensitivity, eye discharge | Dogs become infected by ingesting a tick or prey animal. Not contagious between dogs or to humans. |

Why This Matters: One Tick, Multiple Diseases
One of the biggest challenges with tick-borne illness is the risk of co-infection. A single tick can carry more than one type of bacteria, and dogs exposed to multiple tick species (common in rural or wooded areas, or during travel) may contract more than one disease at the same time. This makes diagnosis more complicated—and treatment more intense.
Some symptoms may overlap or cancel each other out, making it harder for pet owners and even vets to spot the full picture early on. That’s why it’s so important to understand the common signs, use year-round prevention, and work closely with your vet if you suspect anything is off.
In the next section, I’ll walk you through how tick-borne diseases are diagnosed, how treatment works, and what you can expect during recovery—whether your dog has one infection or more than one to fight off.
Diagnosing Tick-Borne Diseases in Dogs
Diagnosis typically begins with a physical exam—your vet may look for ticks or signs of illness like swollen lymph nodes, joint pain, or pale gums. Most cases require blood tests to detect abnormalities such as low platelet counts (thrombocytopenia), anemia, and changes in white blood cell numbers.
In more advanced cases, vets may run urinalysis or imaging (like X-rays or ultrasounds) to assess organ function, especially the kidneys and liver [Cornell University College of Veterinary Medicine]. If tick exposure is recent and symptoms are strong, your vet may begin treatment before test results return.
Treating Tick-Borne Diseases
Fortunately, most tick-borne diseases respond well to a course of antibiotics—most commonly doxycycline, minocycline, or tetracycline. These drugs are broad-spectrum and effective against the majority of the bacterial organisms carried by ticks.
Supportive care can include:
- Anti-inflammatory medications for joint and muscle pain
- IV fluids for dehydration or systemic infection
- Blood transfusions, in cases of severe anemia (more common in babesiosis or ehrlichiosis)
Improvement is often seen within 24–48 hours of beginning treatment, although recovery may take weeks, especially in chronic or multi-infection cases. Long-term complications, such as kidney disease or neurological issues, may still arise depending on the severity and timing of treatment [American College of Veterinary Internal Medicine].
Prognosis: What to Expect
Dogs diagnosed and treated early generally recover well and may even develop immunity to the specific strain they were infected with. However, late-stage or chronically infected dogs may experience long-term effects, including:
- Kidney damage (especially with Lyme disease)
- Eye or neurological complications (ehrlichiosis or Rocky Mountain spotted fever)
- Relapses or lingering fatigue after babesiosis
The sooner treatment begins, the better the outcome. Always trust your gut—if your dog seems “off” after a tick bite, act quickly.
Preventing Tick-Borne Disease: A Year-Round Strategy
Tick-borne illness is unpleasant, expensive, and avoidable. Here’s what you can do to keep your dog safe:
1. Use Tick Prevention All Year Long
Your best protection is regular use of vet-recommended preventives—chewables, topical spot-ons, or collars. No method is 100% foolproof, but they reduce your dog’s risk dramatically [Companion Animal Parasite Council].
2. Do Daily Tick Checks
Even in urban parks, ticks are active. After time outside, run your hands through your dog’s coat, paying attention to:
- Inside and behind ears
- Neck, throat, and under the collar
- Armpits and groin folds
- Between the toes
- Tail base and under the tail
Ticks may be brown, black, or gray and range from pinhead size to grape-sized when engorged.
3. Remove Ticks Safely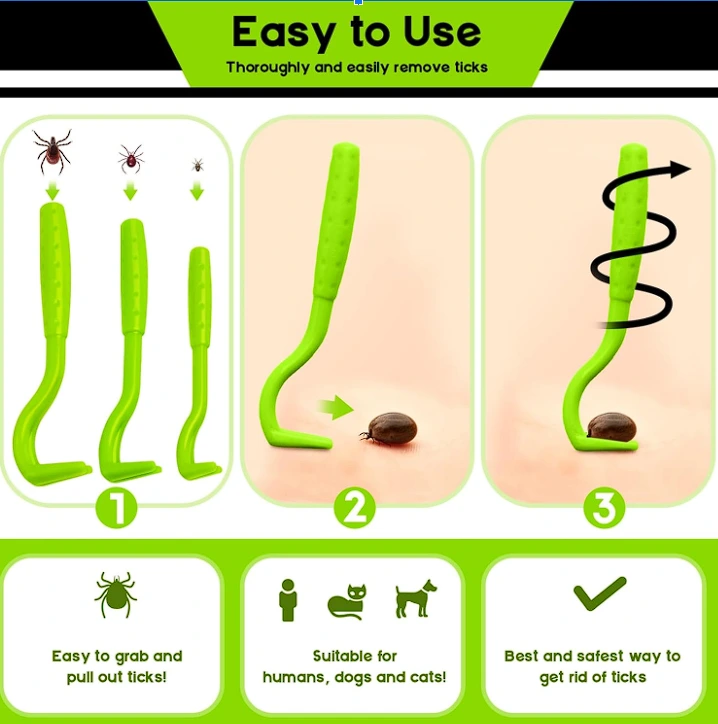
Use tweezers or a tick removal tool. Grab the tick close to the skin and pull gently but firmly. Don’t twist or squeeze—it increases the risk of infection. Dispose of ticks by dropping them in alcohol or flushing them.
4. Maintain a Tick-Unfriendly Yard
- Mow regularly
- Clear leaf piles and tall grasses
- Create gravel or mulch barriers around dog paths or rest areas
5. Use Common Sense in Tick Country
If you’re off-leash hiking in tick-heavy areas, enjoy it—but stay mindful. Dogs don’t live in bubbles, and neither should we. Just be thorough about post-adventure tick checks, for both of you.
Up next: How to build a recovery plan if your dog has been diagnosed with one or more tick-borne diseases—and when to push for additional diagnostics if things aren’t adding up.
Recovery Plan: When the Diagnosis Feels Overwhelming
If your dog has just been diagnosed with a tick-borne disease, especially one picked up abroad—like from a tropical region or rescue situation—it can feel like the bottom just dropped out. I’ve met more than a few well-meaning dog owners who brought home a street dog from Costa Rica or another tropical country, only to face a cascade of unexpected vet bills and symptoms weeks—or even months—later.
Tick-borne diseases often lie dormant or go unnoticed until stress, climate change, or time triggers symptoms. Don’t panic. Here’s a clear and manageable recovery plan to help you navigate the weeks ahead:
🩺 Step 1: Confirm the Diagnosis
Even if the vet has already started antibiotics, it’s important to complete bloodwork to confirm the diagnosis and rule out co-infections. Ask your vet to test for:
- Ehrlichia, Anaplasma, Rickettsia (tick fever), Borrelia (Lyme), and Babesia
- Full CBC and biochemistry panel to assess platelet counts, kidney and liver function
💸 Estimated cost: $250–$400 USD depending on how many tests are run
💊 Step 2: Begin Treatment (and Stick With It)
- Most tick-borne diseases are treated with doxycycline, prescribed for 21–28 days.
- If your dog is vomiting, lethargic, or not eating, your vet may add anti-nausea or anti-inflammatory meds.
- IV fluids or hospitalization may be needed in more serious cases.
- Follow-up bloodwork is often done after treatment to confirm improvement.
💸 Estimated medication and supportive care cost: $100–$600 USD depending on severity
🍖 Step 3: Support Recovery at Home
- Nutrition matters: Feed a high-quality, easily digestible diet.
- Offer small, frequent meals if your dog’s appetite is low.
- Consider probiotics if antibiotics upset your dog’s stomach.
- Restrict heavy exercise during recovery. Allow gentle walks and rest.
💡 Tip: You might not see improvement for a few days—don’t expect an overnight transformation.
📆 Step 4: Schedule Follow-Up Monitoring
Dogs that have had one tick-borne illness are at higher risk for complications or future tick-borne exposures. Set reminders for:
- Follow-up bloodwork 4–6 weeks post-treatment
- Monthly tick prevention (discuss with your vet what’s best for your region)
- Ongoing tick checks, especially after travel or outdoor time
💸 Follow-up testing costs: ~$150–$250 USD per visit
🧳 Special Note for Rescue Dogs from Tropical Regions
If you’ve adopted a dog from Central America, the Caribbean, or the Southern U.S., it’s smart to request pre-adoption screening for tick-borne illnesses—especially if you’re unsure of the dog’s medical history.
Infections like Ehrlichiosis, Anaplasmosis, and Babesiosis are more common in tropical regions and may take weeks or months to become symptomatic. Stress, new climates, and poor nutrition can trigger dormant disease.
Even if the dog seems healthy, keep an eye out for:
- Sudden fatigue or limping
- Nosebleeds or bruising
- Loss of appetite or vomiting
- Swollen joints or lymph nodes
Early treatment makes all the difference.
Make Tick Checks a Daily Habit: Prevention Beyond Medication
One of the best things you can do for your dog—and yourself—is to develop a routine of checking for ticks after outdoor time. This habit became second nature to me when I was training dogs on the tick-heavy grounds of central Kentucky and across the southeastern States. Before we even loaded the dogs back into the truck, every handler was doing a fingertip sweep through fur, toes, ears, and bellies.
And now, living on a rural property, it’s a daily habit. Not just for the dogs, but for me too.
Here’s how to stay ahead of tick-borne diseases with simple daily prevention:
✅ Check Your Dog (and Yourself!) After Every Outing
After a hike, a trail walk, or even time spent in a park or your backyard during tick season:
- Run your fingers through your dog’s fur, feeling for small bumps
- Check key hiding spots: behind ears, under the collar, groin folds, armpits, between toes, under the tail
- Don’t forget your own clothing, hairline, and socks—ticks don’t discriminate
🛠️ Use the Right Tools
- Have a tick remover or fine-tipped tweezers on hand
- Remove the tick close to the skin—no twisting or squeezing
- Drop it in rubbing alcohol or flush it. Never crush a tick with your fingers
🧠 Stay Informed & Be Proactive
- Keep up with your regional tick risk reports (some provinces/states post weekly updates)
- Ask your vet which tick prevention is most effective for your area and your dog’s lifestyle
- If your dog shows any signs of illness after finding a tick, don’t wait—call your vet
A few minutes of prevention each day can save you a ton of heartache (and vet bills) down the road. Whether your dog is running through the Kentucky grasslands or sniffing along a Canadian trail, ticks are opportunists. Be one step ahead.
For information on tick-borne diseases, detection, and treatment visit the PetMD website
💬 Final Thoughts
Tick-borne diseases are scary, yes. But they’re not unbeatable. With good vet care, a watchful eye, and a little patience, most dogs recover well and go on to live full lives.
If you suspect your dog has tick fever, Lyme, or any other tick-borne illness, get them to your vet. The sooner you act, the better their chances.
And if you need help sorting out symptoms, questions, or just want a plan that works for your dog—book a Zoom call with me. You’re not alone in this.
More Information & Trusted Resources
If you want to dive deeper into the science and veterinary knowledge behind tick-borne diseases in dogs, here are some well-regarded, evidence-based resources I’ve referenced or recommend:
📚 Further Reading:
- Cornell University College of Veterinary Medicine – Tick-Borne Diseases in Dogs
https://www.vet.cornell.edu - American College of Veterinary Internal Medicine (ACVIM) – Infectious Disease Guidelines
https://www.acvim.org - Companion Animal Parasite Council (CAPC) – Tick Prevention & Disease Prevalence Maps
https://capcvet.org - Merck Veterinary Manual – Canine Tick-Borne Diseases Overview
https://www.merckvetmanual.com - Centers for Disease Control and Prevention (CDC) – Tick-Borne Diseases of the United States
https://www.cdc.gov/ticks/diseases
These sources are helpful whether you’re a curious owner, a first-time adopter, or just trying to make sense of your vet’s diagnosis. I always recommend staying informed—it’s the best defense we have.
✅ Bonus Resource:
Want a quick-reference guide to stay one step ahead of ticks?
[Download our Tick Prevention & Daily Check Checklist here.]
Enjoyed this read? For more no-nonsense insights on dog training and behavior, check out my earlier blogs:
• Dog Rescue in Costa Rica: How It’s Different from the West
• Street Dogs and Freedom: The Hidden Side of Canine Happiness
There’s always something new to learn, even if it’s just a different perspective on the everyday challenges we face. Happy reading!
Join my Email List to get frequent updates, free downloadables, and dog training tips! Click here to subscribe.
Get the latest updates when we publish new freebies and guides by signing up. Your dog will thank you, and you’ll be the first to know when new gifts are available!
Let’s stay connected:

